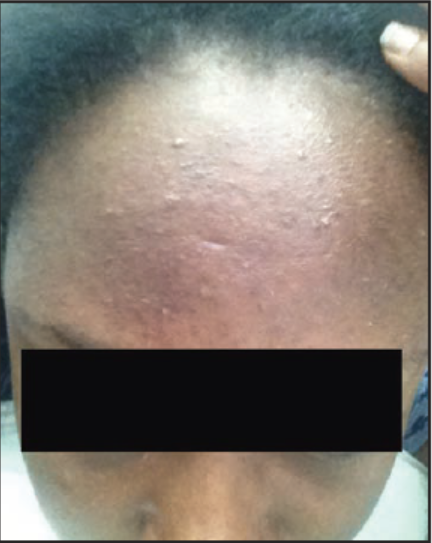
I later discovered that I may have had another skin condition called Pityrosporum Follicultitis, a skin condition caused by infection by pityrosporum yeast. To treat it, a doctor put me on a short-term course of prescription antifungal medication. To date, the forehead minefield has not returned (fingers crossed!). So, what do you do if you also suffer from particularly stubborn acne that will not respond to any acne treatment you try? Review the list of acne look-alikes below to determine if your acne might actually be another condition.
Pityrosporum Folliculitis (also called “Malassezia Folliculitis”)
According to a 2014 case report from the Journal of Clinical and Aesthetic Dermatology, Pityrosporum folliculitis was first recognized as a specific disease in 1973 (the full case review is very informative (pdf)). Commonly misdiagnosed as acne vulgaris, Pityrosporum folliculitis is a fungal condition that results from an overgrowth of the Malassezia yeast present in the normal cutaneous flora. The yeast is found in the sebaceous glands, as it thrives on the lipid composition of sebum.
The condition is most often located on the chest, back, posterior arms, and face. It is commonly found in people living in hot, humid climates, particularly those affected by excessive sweating. Pityrosporum folliculitis is most common in males. Additionally, the condition often affects those who have a history of topical or oral antibiotic use, particularly tetracyclines, oral corticosteroid use, and immunosuppression. One indication of the disease is the drastic improvement following use of antifungal medications. Note that use of antibiotics can worsen the condition by altering normal flora and leading to the yeast’s overgrowth. Tetracyclines for acne, in particular, can actually worsen yeast infections.
Symptoms: Pityrosporum folliculitis typically appears as small, non-inflamed bumps that show up on the forehead. Folliculitis extracts much differently than an acne lesion (the pustules are pus-filled). It tends to be quite itchy, and the bumps may appear more prominent when scratched.
Treatments: In the aforementioned study, Pityrosporum folliculitis was treated with a course of antifungal medication (specifically, oral fluconazole 100mg daily), topical clotrimazole cream applied twice daily, and tretinoin 0.0375% cream.
Miliaria
Also called heat rash, miliaria is marked by small red bumps that have white heads. Miliaria occurs after strenuous exercise and frequently itches. Heat rash usually clears on its own, but return if hot, humid weather persists. And though it is common in newborns, adults can develop it, too. Keep the area cool and dry.
Symptoms: Lesions appear in crops within days to weeks of exposure to hot weather and disappear within hours to days.
Treatment: The prevention and treatment of miliaria primarily consists of controlling heat and humidity so that sweating is not stimulated. Topical treatments that have been advocated involve lotions containing calamine, boric acid, or menthol; cool wet-to-dry compresses; frequent showering with soap (although some medical professionals discourage excessive use of soap); topical corticosteroids; and topical antibiotics.
Keratosis Pilaris
Keratosis pilaris is a common skin condition that causes rough patches and small, white (and sometimes red) acne-like bumps, usually on the arms, thighs, cheeks and buttocks. Unlike Miliaria and Pityrosporum folliculitis, Keratosis pilaris generally does not hurt or itch.
Symptoms: Small white or red bumps, typically on the upper arms, legs, buttocks or cheeks.
Treatment: According to Dr. Jessica Wu, using a body scrub twice a week and then applying a rich cream can soften the plugged hair follicles (see “Feed Your Face”). Medicated creams containing alpha-hydroxy acid, lactic acid, salicylic acid or urea moisturize and soften dry skin while helping to loosen and remove dead skin cells.
Perioral Dermatitis
Perioral dermatitis is a common facial skin problem in which groups of itchy or tender small red papules (bumps) appear around the mouth. The papules spare the skin bordering the lips (which then appears pale) but develop on the sides of the chin, and then spread to include upper lip and cheeks. The surrounding skin may be pink, and the skin surface often becomes dry and flaky. Periorificial dermatitis is the name used for the same disorder when it spreads to sites other than around the mouth (Periorificial dermatitis can spread to the nose area, on the eyelids and around the eyes, on or around genital skin, or around the anus).
The exact cause of perioral dermatitis is not understood; it is thought to be a variant of rosacea, which is now known to be due to a complex activation of the innate immune system. The rash may be induced by neglecting to wash the face, certain cosmetics, topical steroid creams, nasal steroids and steroid inhalers and fluorinated toothpaste. Perioral dermatitis may be related to an imbalance of, or immune reaction to, proliferating bacteria and yeasts in the hair follicles.
Symptoms: Small red papules (bumps) appear around the mouth.
Treatment: Discontinue applying all face creams including topical steroids, cosmetics and sunscreens
Wash the face with warm water alone while the rash is present. When it has cleared up, use a non-soap bar or liquid cleanser if you wish.
Rosacea
Rosacea is a common skin condition that causes redness in the face and often produces small, red, pus-filled bumps. Although rosacea can occur in anyone, it most commonly affects fair-skinned middle-aged women.
Symptoms: Rosacea usually causes a persistent redness in the central portion of your face. Small blood vessels on your nose and cheeks often swell and become visible. Rarely, rosacea can thicken the skin on the nose, causing the nose to appear bulbous (rhinophyma).
Treatment: Wear broad-spectrum sunscreen with an SPF of 30 or higher. Avoid spicy foods and try not to irritant your facial skin by rubbing or touching it too much.